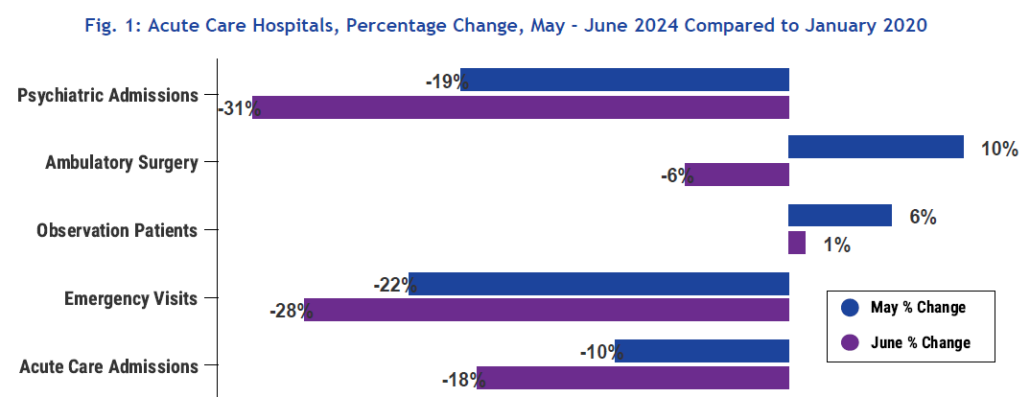July 2024 Utilization Report
يسلط الضوء
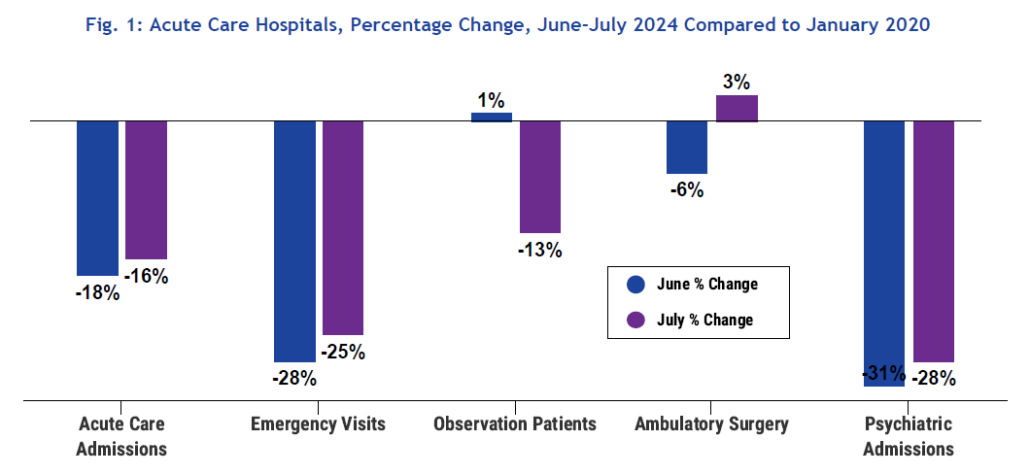
All except one of the focus utilization metrics saw an increase in volumes going from June to July 2024 compared to 2020 pre-COVID baselines. Ambulatory surgeries present the biggest jump in numbers going from -6% below the baseline in June, to 3% over the baseline in July. Comparably, acute care admissions changed going from -18% below the baseline in June to -16% in July, Emergency Department visits went from -28% to -25%, and psychiatric admissions increased in volumes going from -31% in June to -28% in July. Observation admissions is the sole metric with declining volumes going from 1% above baseline in June to -13% in July (see Fig.1 below).
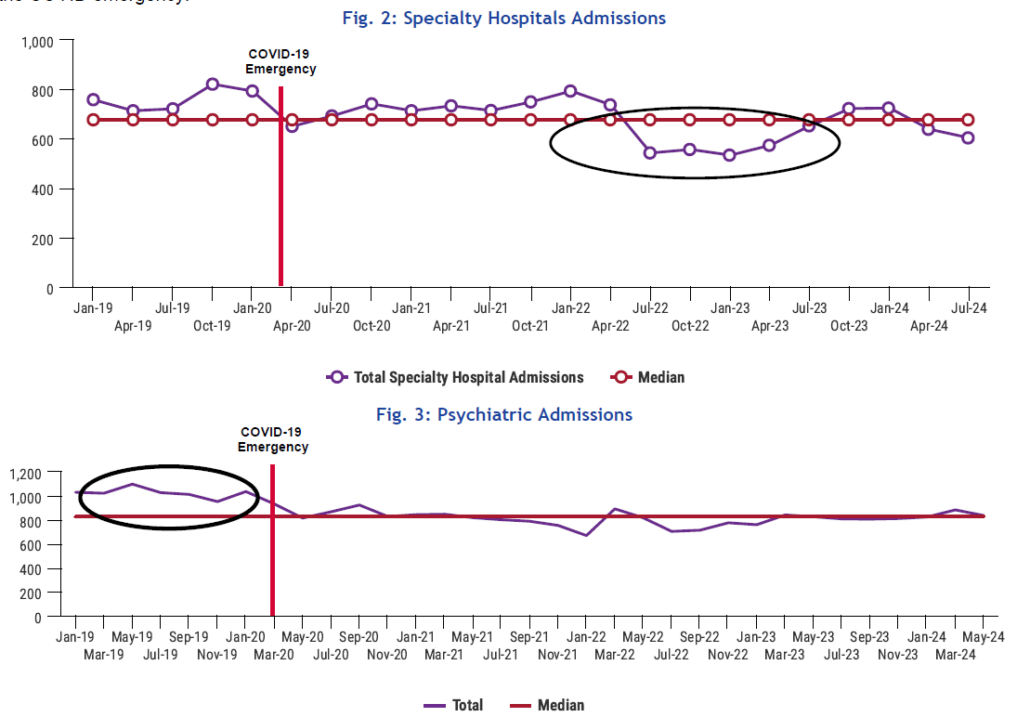
Looking at observation admissions it is important to note that although there has been less variation over the past few months and volumes have recovered compared to the height of the pandemic, recent volumes have decline and gone below the median this month as shown in Fig. 2.